Key Insights from My Curated Resources on Determinants of Health
- Oct 11, 2023
- 3 min read
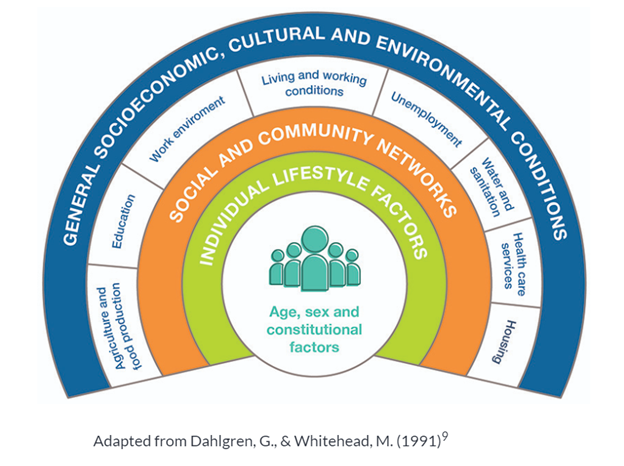
The overall health and well-being of any person are influenced by a combination of interconnected factors, not solely by what we eat or how much we exercise. Each individual has unique circumstances, such as genetics, environment, socioeconomic status, and access to health services, that define their health (World Health Organization, 2017). Collectively, the factors and circumstances affecting someone’s health are known as determinants of health. Some of these determinants are beyond the person’s control. Where we live, our environment, genetics, income, education, and relationships significantly influence our health, while access to healthcare, which receives more focus, tends to have a smaller impact (World Health Organization, 2017). Under the broader umbrella of determinants of health, factors such as home country, income, housing, education, work, food, and social support networks are categorized under the social determinants of health (SDH). Better SDH promotes health equity as “health and illness follow a social gradient: the lower the socioeconomic position, the worse the health” (World Health Organization, n.d.).
The federal government of Canada lists the 12 main determinants of health, including factors such as income, childhood experiences, healthy behaviours, biology, and race, among others, as the determinants of citizens’ health (Public Health Agency of Canada, 2023). From this list, the social and economic factors that pertain to the person’s place in society are called SDH. Historical trauma and racism are significant SDH for certain groups in Canada. These factors contribute to health inequalities, and it's important to recognize that the health of these groups is influenced by more than just personal choices and genetics (Public Health Agency of Canada, 2023). According to Alberta Health Services (n.d.), “There are 3 basic levels to target when looking to improve people’s health and wellness: individual, community and policy.” The first to draw attention is the individual level, where actions such as exercising, eating healthy and quitting smoking improve health outcomes. However, the community level, which involves creating healthy environments, and the policy level, through the implementation of healthy policies, requires active monitoring and continuous improvement. These two levels have a significant impact on SDH. When dealing with symptoms of health inequities, we need to “think upstream” to create conditions for all citizens to enjoy true health (Upstream, 2013).
An example of innovation and thinking upstream is the idea of utilizing the significant potential of paramedics to address SDH to reduce the strain on the healthcare system and emergency departments. In Canada, community paramedicine programs currently target a limited patient population, with less than 20% involving unscheduled calls. This results in only a limited number of community paramedics assessing for SDH and addressing them while treating a relatively small number of patients (Allana & Pinto, 2021). Paramedics, with enhanced practice in social and environmental assessments, may refer patients to primary care teams and community-based organizations or social workers, to address SDH (Allana & Pinto, 2021). Equipping paramedics with enhanced tools, criteria, and questionnaires to assess patients for housing, income, and food security risks and addressing them promotes care continuity. However, fully enabling this initiative requires changes in education, culture, and governance. This approach can help alleviate strain on the secondary care system and enhance the well-being of individuals, especially in vulnerable or older adult communities (Allana & Pinto, 2021).
Health and health equity are fundamental human needs. By defining determinants of health at global, federal, and provincial levels, improvements can be made to enhance individual, community, and policy levels of determinants, promoting upstream thinking. Creative strategies, such as utilizing frontline healthcare providers like community paramedics to assess and address SDH, exemplify upstream thinking. Nonetheless, realizing this potential requires funding and intentional policy changes to fully enable such initiatives and to promote health equity in a fast-changing landscape.
References
Alberta Health Services. (n.d.). What determines health? Alberta Health Services. https://albertahealthycommunities.healthiertogether.ca/about/what-determines-health/
Allana, A., & Pinto, A. D. (2021). Paramedics Have Untapped Potential to Address Social Determinants of Health in Canada. Healthcare Policy, 16(3), 67–75. https://doi.org/10.12927/hcpol.2021.26432
Public Health Agency of Canada, G. of C. (2023, June 1). Social determinants of health and health inequalities [Policies]. https://www.canada.ca/en/public-health/services/health-promotion/population-health/what-determines-health.html
Upstream. (2013, September 25). Introduction to Upstream. [Video]. YouTube. https://www.youtube.com/watch?v=qarQXqKbmLg
World Health Organization. (n.d.). Social determinants of health. https://www.who.int/health-topics/social-determinants-of-health
World Health Organization. (2017). Determinants of health. https://www.who.int/news-room/questions-and-answers/item/determinants-of-health



Comments